FEPP Fit:
An exercise/lifestyle intervention for young adults with schizophrenia.
Many individuals with schizophrenia spectrum disorders (SSDs) have physical health problems, such as high blood pressure, diabetes, obesity, and high cholesterol, as well as high rates of health damaging behaviors, such as smoking and physical inactivity. These risk factors are present for young persons with SSDs, suggesting that they should be a focus of treatment early in the course of illness. Research has shown that lifestyle interventions, such as those involving exercise and nutrition counseling, can be helpful for improving physical and mental health among persons with SSDs. Yet, there have been few programs developed specifically for young adults with SSDs, and of those that have been tested, many do not result in continued exercise and/or healthy nutrition once the program ends.
PROJECT STATUS
Browne J, Cather C, Zvonar V, Thayer K, Skiest H, Arntz D, Kritikos K, Schnitzer K, Brown HE, Evins AE, Donovan AL. Developing a sound body: Open trial results of a group healthy lifestyle intervention for young adults with psychosis. Community Mental Health Journal. 2020.
AIMS
This study tested a new exercise/lifestyle intervention, “FEPP Fit,” in a sample of young adults with SSDs. The aims of the study were to evaluate: 1) feasibility (i.e. how likely people were to participate in the program via attendance rates and satisfaction ratings) and 2) the effect the program had on self-reported hours spent sitting and steps per day (measured with pedometers), nutritional knowledge, weight, resting heart rate, waist-hip ratio, and well-being (depressive symptoms and overall self-reported health and memory) at the end of program and 11 weeks later.
METHODS
Sixteen participants with SSDs enrolled in an 11-week study of “FEPP Fit,” which included group exercise sessions and group health/wellness education sessions. The 60-minute group exercise sessions were run by a trainer at a local gym and followed a high-intensity interval training program, which included a warm-up, intervals of strength and aerobic exercises, cool-down, and stretching.
FEPP Fit Exercise Sessions

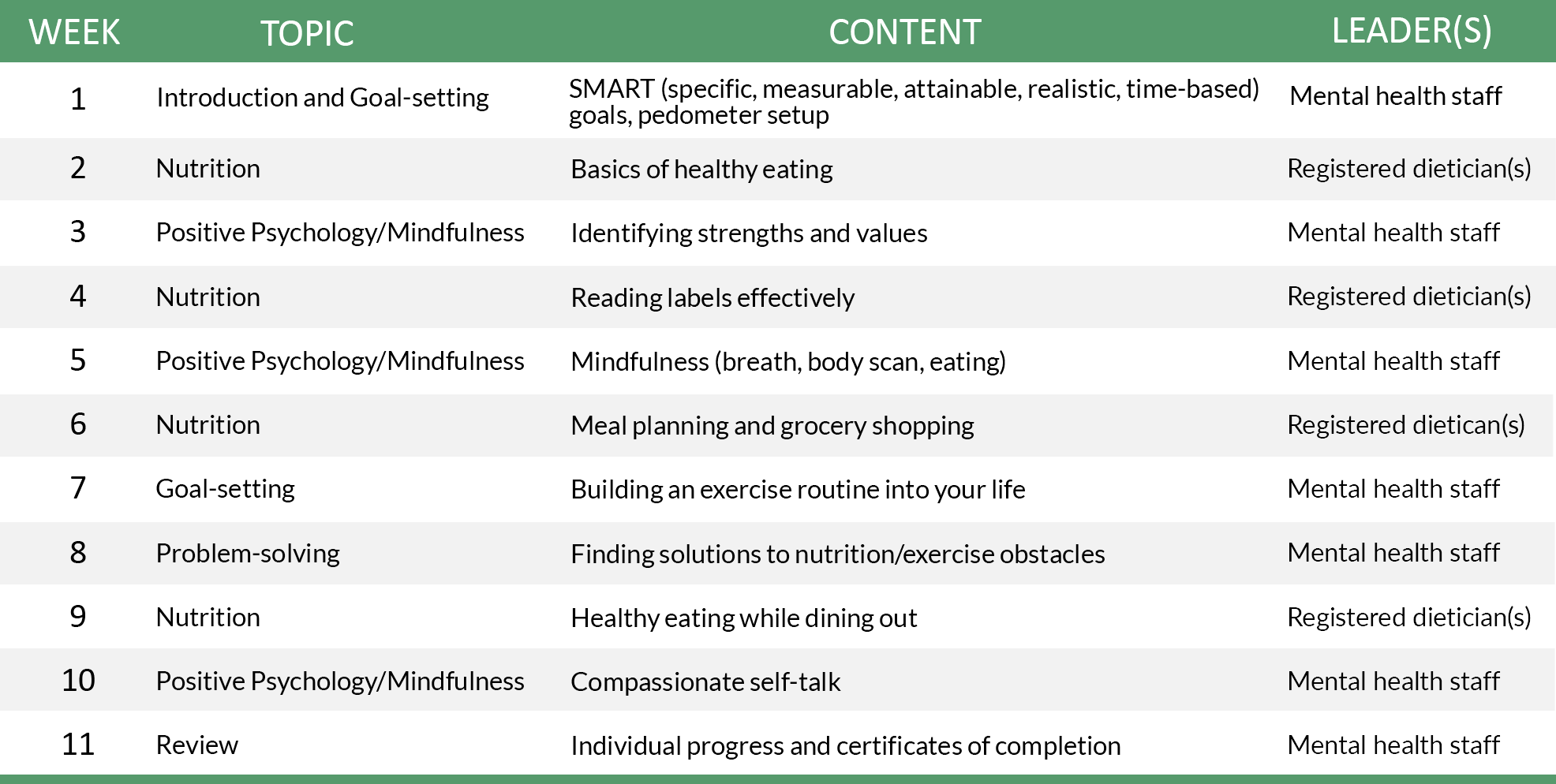
The health and wellness education sessions, run by nutritionists and mental health staff, focused on learning about nutrition, setting weekly nutrition goals, using a pedometer to measure daily steps, problem-solving, and promoting positive psychology/mindfulness. Groups were held once a week (exercise followed by health and wellness education) for 11 weeks, and participants could earn $3.00/week, if they attended both sessions. Participants were encouraged to wear their pedometer every day to track steps, and they completed measures of physical health and mental health before the intervention started, after it ended (11 weeks), and 11 weeks after it ended.
FEPP Fit Wellness Education
RESULTS
Attendance rates were 73% for the exercise groups and 70% for the health and wellness education groups. Participants also reported high levels of satisfaction with FEPP Fit. Together, these results suggest that the intervention was feasible and well-received by participants. In terms of hours spent sitting and steps per day, results showed that participants walked an average of 2,300 more steps during the intervention period and lowered how much they were sitting from approximately eight hours/day before the intervention to approximately seven hours/day after the intervention ended to approximately six hours per day 11 weeks after the intervention ended. These results show that FEPP Fit resulted in more physical activity and less sitting time, which are both important to improving physical health and quality of life. Results did not demonstrate meaningful changes in other measures.

Overall, this study tested a new lifestyle intervention, FEPP Fit, in a sample of young adults with SSDs, and it demonstrated high attendance rates and satisfaction scores, as well as meaningful increases in physical activity.
COE PROJECT STAFF

Abigail Donovan, MD
PRINCIPAL INVESTIGATOR

Corinne Cather, PhD
CO-INVESTIGATOR

Eden Evins, MD, MPH
CO-INVESTIGATOR

Katherine Kritikos, MPH
PROGRAM MANAGER

Diana Arntz, PhD
RESEARCH FELLOW

Julia Browne, PhD
RESEARCH FELLOW

Hannah Skiest, BA
CLINICAL RESEARCH COORDINATOR

Vanya Zvonar, BA
CLINICAL RESEARCH COORDINATOR
Additional collaborators
Hannah Brown, MD; Kristina Schnitzer, MD; Katherine Thayer, LICSW, MBA.
Funding
Funding for this project was provided by the MGH COE/Massachusetts Department of Mental Health.